Understanding Epilepsy Main Menu
Table of Contents:
- Classification of Seizures and Epilepsy
- Types of Seizures
- Diagnosing Seizures
- Expanded Characteristics of Seizure Types
Classification of Seizures and Epilepsy
The International League Against Epilepsy (ILAE) is a professional organization dedicated to ensuring that healthcare professionals, patients, and their care providers across the world have the educational and research resources that are essential in understanding, diagnosing, and treating people with epilepsy.
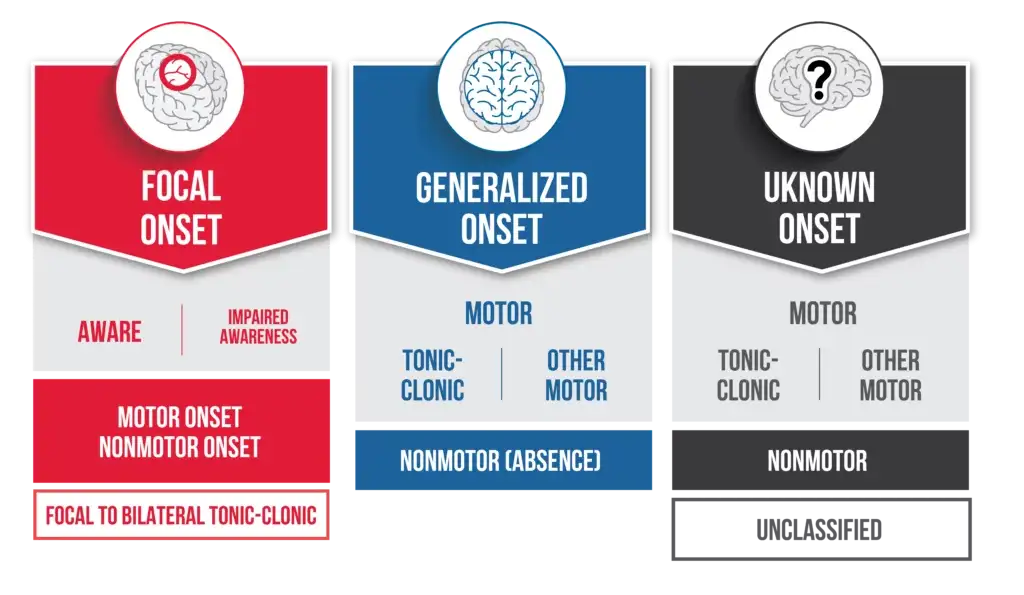
The ILAE has established the terminology and approaches for classifying seizures and forms of epilepsy. This framework, called Classification of the Epilepsies, is the key international resource that healthcare professionals use when diagnosing and treating patients with epilepsy. The ILAE updated the Classification of the Epilepsies in 2017, resulting in new, more accurate names for seizures, and takes the following into account: [1], [2]
- Seizure onset (does it have a generalized or focal or onset?)
- Additional features (is there a physical component? Is awareness impaired?)
- Expanded classification (what other symptoms occur along with the seizure?)
Seizures are first classified by their onset. This is the initial and most basic identification of seizure type under the new system. Any further classification by looking at awareness during a focal seizure, motor/nonmotor onset, and the features of the seizure is optional.
Types of Seizures
There are several different types of seizures, each with its own distinct characteristics and symptoms. The main types of seizures include:
Focal Onset Seizures
Formerly known as “partial” seizures, focal seizures start on one side, also known as a hemisphere, of the brain. This type of seizure affects approximately 60% of people with epilepsy.2-4 Focal seizures can be divided into different types based on whether consciousness is impaired during the event.2
Generalized Onset
Generalized seizures involve both hemispheres of the brain. These seizures can have a physical component, such as a fall or muscle contraction (ex. jerks), or they may have no physical component (absence seizure).2
Unknown Onset
In some cases, the beginning of a seizure is not entirely known. This may be because the person was alone when the seizure occurred, or because diagnostic testing has not yet been conducted and there is inadequate information to make the identification.
Once the physician knows how and where the seizure started, a person’s seizures are classified. However, there is an opportunity for seizure’s name to be more descriptive by including additional information – that’s where additional features come in.
Focal to Bilateral
There are also times when a seizure begins in one hemisphere of the brain and then spread to the other side of the brain. These seizures are referred to as bilateral.
Diagnosing Seizures
The next step in classifying seizures involves looking at additional features that occurred with the seizure. While this step is optional, doing so allows the physician to include some additional information about the type of seizure by looking at a couple of characteristics:
- For focal, generalized, and unknown onset seizures, are there motor behaviors (i.e. was there movement involved at the start of the seizure) or nonmotor characteristics (i.e. sensory experiences, such as smelling or tasting something)?
- For focal seizures, is awareness impaired (i.e. a loss of consciousness) at any time during the seizure?
- Does the seizure originate as a focal seizure but then spread to both hemispheres of the brain (formerly known as secondarily generalized)?
ILAW 2017 Classification of Seizure Types
Focal onset seizures can be further divided by whether a person is or is not aware of their surroundings during the seizure:
- Focal onset with retained awareness seizures (focal aware): the person is aware of their surroundings throughout the seizure
- Focal onset with impaired awareness seizures (focal unaware): the person is not aware of their surroundings at any point during the seizure
- Focal onset awareness unknown: it is not known if the person loses awareness or not (ex. if the person lives alone, or if their seizures occur only at night)
Awareness is reflecting on whether the person seizing had any knowledge of self and the environment during the seizure. It is NOT referring to whether or not the individual was aware that a seizure had occurred. If awareness of the seizure is impaired for any portion of it, then the seizure is classified as focal unaware.
Since most generalized seizures involve loss of consciousness, there is no additional descriptor on awareness used with generalized seizures.
Answering these questions is important because it helps the diagnosing physician more descriptively characterize the type of seizure that occurred.
Expanded Characteristics of Seizure Types
The 2017 seizure classification system allows for an even greater description of the seizure beyond the characterizations explained in the section above. It provides more detailed information on the level of motor and nonmotor symptoms seen with the seizures.
Focal onset seizures
Focal onset seizures can be further classified into seizures that have a physical component (motor) and those that do not have a physical component (nonmotor).
Focal Motor Seizures
- Atonic seizures or “drop” seizures consisting of sudden loss of muscle tone (i.e. the person may fall unexpectedly)
- Automatisms consisting of involuntary, repetitive movements, such as tapping, pacing, or chewing
- Clonic seizures consisting of repetitive jerking or twitching
- Epileptic Spasms consisting of sudden muscle flection or extension
- Hyperkinetic seizures consisting of limb and socket movements, such as arms and hips (i.e. the person may rock back and forth, jump, or thrash)
- Myoclonic seizures consisting of short, jerking movement of muscles resembling muscle spasms
- Tonic seizures characterized by sudden stiffness and rigidity of muscles
Focal Nonmotor Seizures
- Autonomic seizures which impact involuntary functions, and may disrupt blood pressure, heart rhythm, or bladder function
- Behavior arrest in which movements stop all together
- Cognitive seizures which impairs all cognitive function
- Emotional seizures which can alter mood or emotion, or can give the appearance of an emotion without feeling it
- Sensory seizures which include sensations at the seizure onset, such as feeling a numbness or tingling, or smelling an unpleasant odor
Generalized onset seizures
Generalized onset seizures can be further classified into seizures that have a motor or nonmotor component, as well.
Generalized Motor Seizures
- Atonic seizures or “drop” seizures consisting of sudden loss of muscle tone (i.e. the person may fall unexpectedly)
- Clonic seizures consisting of repetitive jerking or twitching
- Tonic seizures characterized by sudden stiffness and rigidity of muscles
- Myoclonic seizures consisting of short, jerking movement of muscles resembling muscle spasms
- Tonic-clonic seizures (previously called grand-mal) consisting of sudden stiffness (tonic) and repetitive jerking (clonic)
Generalized NonMotor Seizures
- Typical absence seizures occur when the affected person stop what they are doing and stare into space. Sometimes, their eyelids may start fluttering. These seizures are short (about 10 seconds in duration)
- Atypical absence seizures are longer than typical absence seizures. In addition to staring, there can be symptoms such as lip-smacking and repetitive hand movements such as wringing
- Eyelid myoclonia which consists of brief twitches of the eyelid
Psychogenic Non-Epileptic Seizures
Psychogenic non-epileptic seizures (PNES) happen when a person experiences symptoms similar to those of epilepsy, but without any abnormal activity in the brain. The causes of non-epileptic seizures are not fully understood, but non-epileptic seizures may be associated with anxiety, depression, and personality disorders.5 There is also a link between post-traumatic stress disorder (PTSD) and non-epileptic seizures.[5]
Febrile Seizures
A febrile seizure is a type of seizure caused by a fever. This kind of seizure can happen in otherwise healthy children. Febrile seizures typically happen between six months and five years old. Febrile seizures can occur in up to 5% of all children when they have a fever.
Typically, febrile seizures in a child are not life-threatening. They also do not usually indicate a more serious health condition, such as epilepsy. Even so, febrile seizure can be scary and difficult to understand for caregivers and kids. Knowing about potential causes, symptoms, and what to do can help.
Keep Learning
Subscribe to our emails for more content like this.
More about types of seizures
References:
- Scheffer IE, Berkovic S, Capovilla G, Connolly MB, French J, Guilhoto L, et al. ILAE classification of the epilepsies: Position paper of the ILAE Commission for Classification and Terminology Epilepsia. 2017 Apr;58:512-521.
- Fisher RS, Cross JH, D’Souza C, French JA, Haut SR, Higurashi N, et al. Instruction manual for the ILAE 2017 operational classification of seizure types Epilepsia. 2017 Apr;58:531-542.
- Beghi E. The Epidemiology of Epilepsy Neuroepidemiology. 2020;54:185-191.
- The Epilepsies and Seizures: Hope Through Research. Available at: https://www.ninds.nih.gov/Disorders/Patient-Caregiver-Education/Hope-Through-Research/Epilepsies-and-Seizures-Hope-Through.
- Perez DL, LaFrance WC, Jr. Nonepileptic seizures: an updated review CNS Spectr. 2016;21:239-246.